Welcome To Bwindi Community Hospital We treat, God heals
We are a not-for-profit community hospital under the auspices of the Church of Uganda in the Diocese of Kinkiizi. We offer preventative and curative services to 120,000 people, while our specialized services benefit patients nationwide.
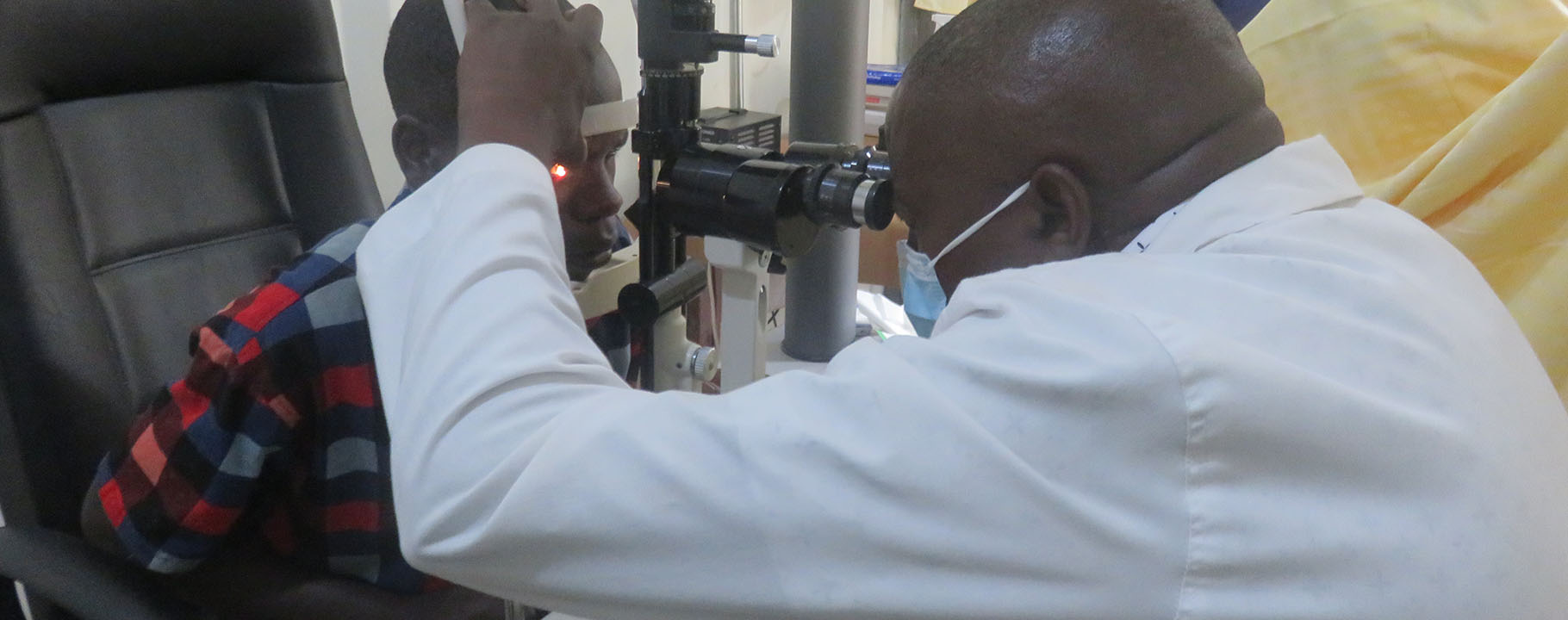
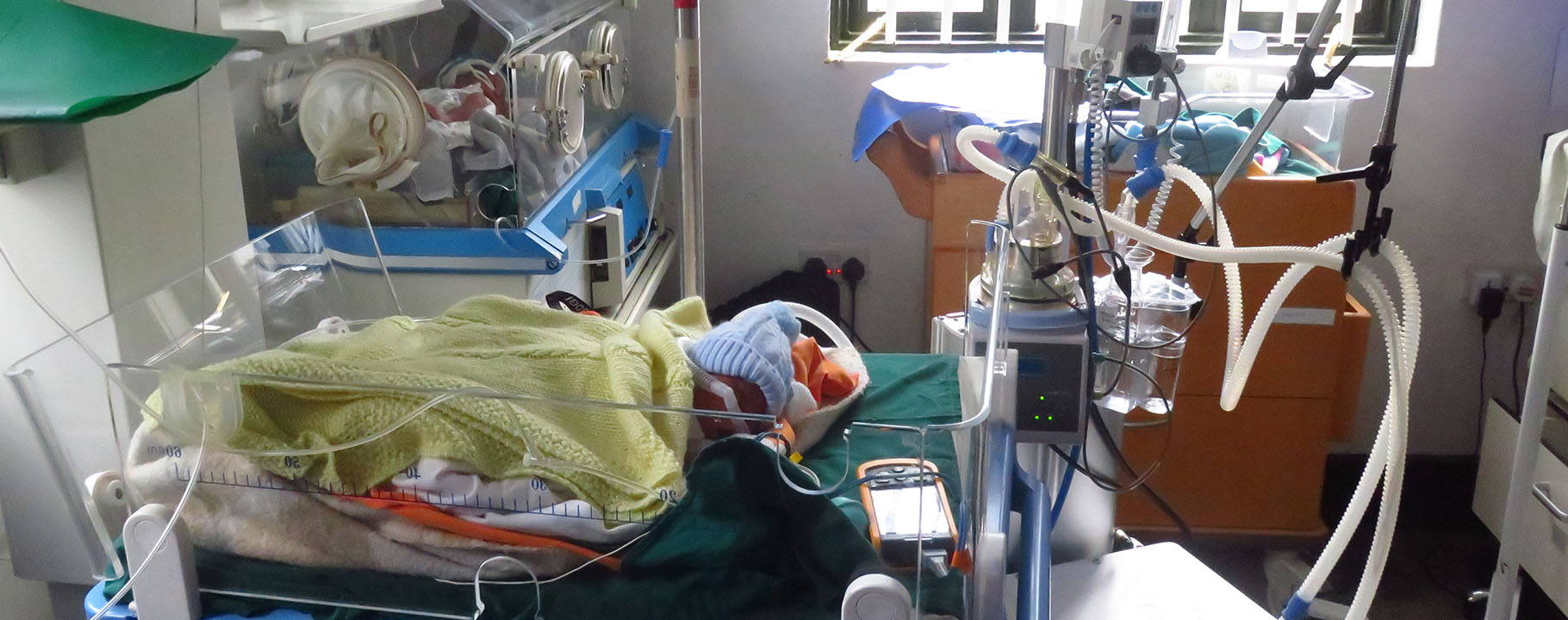
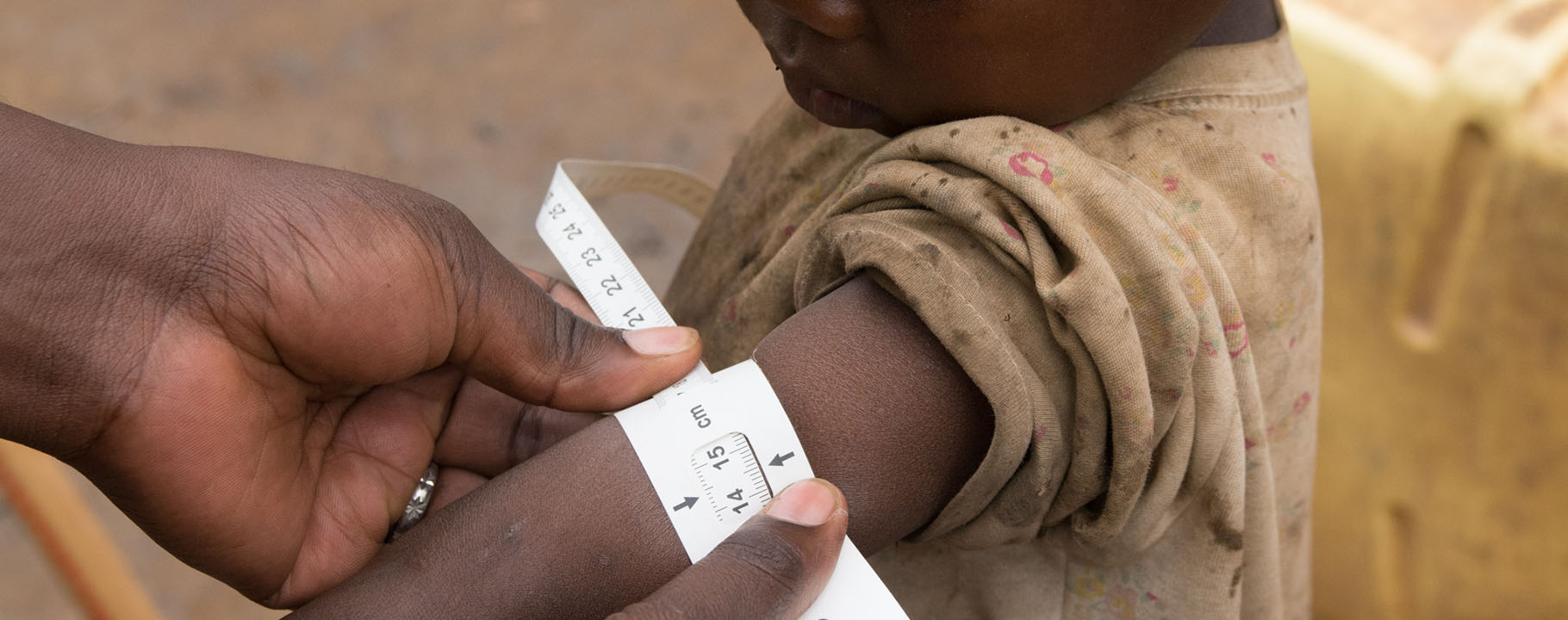
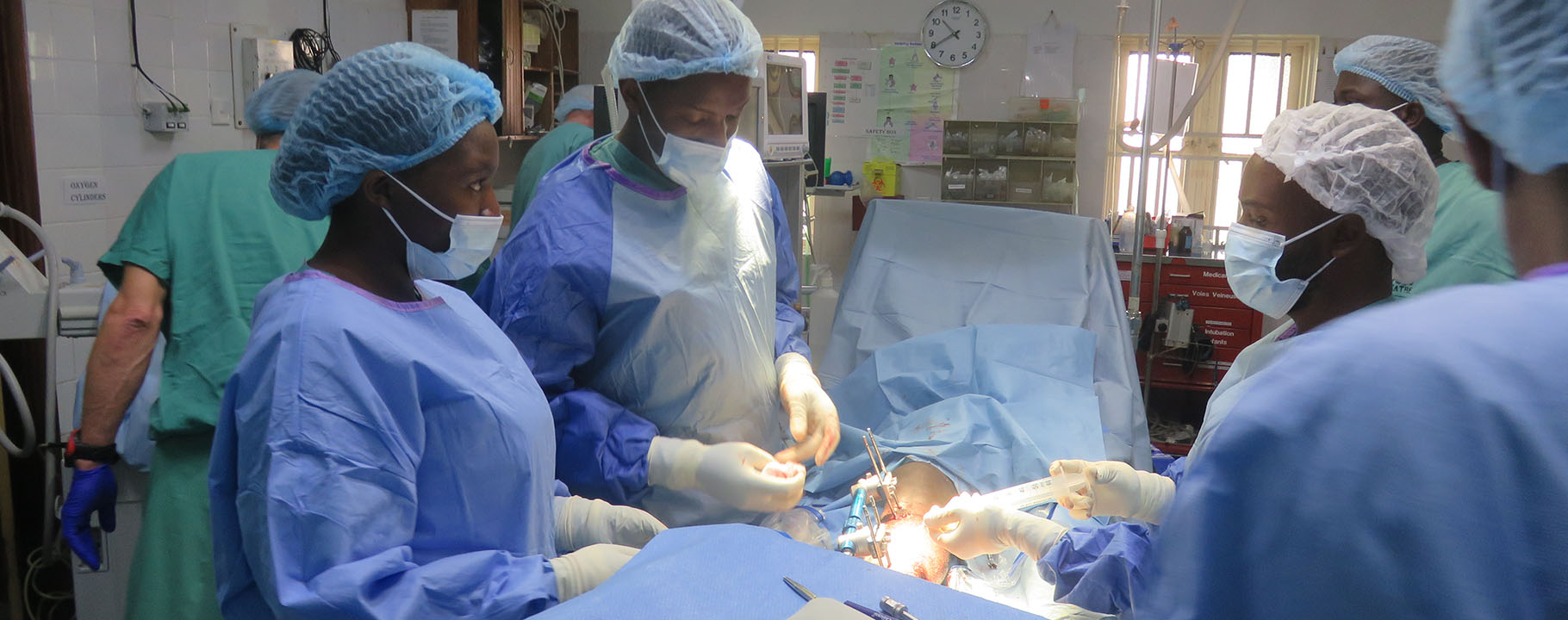
Bwindi Community Hospital (BCH) has a bed capacity of 155 beds and handles about 40000 consultations annually. We provide a wide range of services, including: Outpatient and Inpatient, Child health, Maternal health, Community health and Batwa, Dental and Eye health care, Diagnostics and Laboratory services, Mental health,Chronic Care, Accident and Emergency Services, Ambulance services, HIV/AIDS and TB care, Youth friendly services and eQuality Health Insurance. We also train the next generation of healthcare professionals at Uganda Nursing School Bwindi and Uganda College of Health Sciences Bwindi.
For the last ten years, BCH has consistently ranked among the best-performing health facilities in Uganda, according to the Uganda Protestant Medical Bureau (UPMB).
2024: UPMB Best Quality Service Delivery Award 2024 for embracing ICT in healthcare
2024: Heroes in Health Award 2024, in recognition of the exceptional achievements and dedication to the field of healthcare in the use of ICT to Improve Patient Care Award
2024: Heroes in Health Lifetime Achievement Award 2024 to Dr. Scott Kellermann, in recognition of his outstanding contributions and dedication to improving the well-being of individuals and communities.
2021: Prince Albert II of Monaco Prize for Innovative Philanthropy, in recognition of the exceptional work carried out by BCH to provide access to healthcare for the poorest communities.
2018: UPMB award for innovatively growing the Community Health Insurance, overall best performer in timely compilation and submission of quality reports and good Monitoring and Evaluation practices. .
2018: UPMB award for leading innovation and use of technology in nursing education in Uganda.
2018: Won Social Innovation in health Initiative award by Makerere University School of Public Health for pioneering Mothers Waiting Hostel for safe motherhood in Uganda, as an affordable and sustainable innovation to improve facility deliveries.
2017: Won Grand Challenge Canada innovation Award for using digital and mobile technology to create an affordable community-rooted community health service for poor remote setting.
2017: Winner of the 2017 Uganda sustainable development award by Public Opinions.
2014: Mama Alive Initiative Award (Uganda) for improving maternal health in the region
2013: Public Opinion Pearl of Africa Life Time Achievement Award for contributing towards attainment of the millennium Development goals.
2011: Stars Foundation (UK) health impact ward for Africa and Middle East region for improving child health.
A number of other health facilities from across the country continue to visit Bwindi to learn from our innovations and best practices to help improve healthcare delivery in their own regions.